Immunology
Citation Information: JCI Insight. 2024;9(14):e178767. https://doi.org/10.1172/jci.insight.178767.
Abstract
Radiation therapy (RT) is frequently used to treat cancers, including soft-tissue sarcomas. Prior studies established that the toll-like receptor 9 (TLR9) agonist cytosine-phosphate-guanine oligodeoxynucleotide (CpG) enhances the response to RT in transplanted tumors, but the mechanisms of this enhancement remain unclear. Here, we used CRISPR/Cas9 and the chemical carcinogen 3-methylcholanthrene (MCA) to generate autochthonous soft-tissue sarcomas with high tumor mutation burden. Treatment with a single fraction of 20 Gy RT and 2 doses of CpG significantly enhanced tumor response, which was abrogated by genetic or immunodepletion of CD8+ T cells. To characterize the immune response to CpG+RT, we performed bulk RNA-Seq, single-cell RNA-Seq, and mass cytometry. Sarcomas treated with 20 Gy and CpG demonstrated increased CD8 T cells expressing markers associated with activation and proliferation, such as Granzyme B, Ki-67, and IFN-γ. CpG+RT also upregulated antigen presentation pathways on myeloid cells. Furthermore, in sarcomas treated with CpG+RT, TCR clonality analysis suggests an increase in clonal T cell dominance. Collectively, these findings demonstrate that CpG+RT significantly delays tumor growth in a CD8 T cell–dependent manner. These results provide a strong rationale for clinical trials evaluating CpG or other TLR9 agonists with RT in patients with soft-tissue sarcoma.
Authors
Chang Su, Collin L. Kent, Matthew Pierpoint, Warren Floyd, Lixia Luo, Nerissa T. Williams, Yan Ma, Brian Peng, Alexander L. Lazarides, Ajay Subramanian, Jonathon E. Himes, Vincent M. Perez, Rosa D. Hernansaiz-Ballesteros, Kimberly E. Roche, Jennifer L. Modliszewski, Sara R. Selitsky, Mari L. Shinohara, Amy J. Wisdom, Everett J. Moding, Yvonne M. Mowery, David G. Kirsch
Citation Information: JCI Insight. 2024. https://doi.org/10.1172/jci.insight.182312.
Abstract
We evaluated the safety and viral rebound, after analytical treatment interruption (ATI), of vedolizumab and ART in recent HIV-1 infection. We used this model to analyze the impact of α4β7 on the HIV-1 reservoir size. Participants started ART with monthly Vedolizumab infusions and ATI was performed at week 24. Biopsies were obtained from ileum and caecum at baseline and week 24. Vedolizumab levels, HIV-1 reservoir, flow cytometry and cell-sorting and antibody competition experiments were assayed. Vedolizumab was safe and well-tolerated. No participant achieved undetectable viremia off ART 24 weeks after ATI. Only a modest effect on the time to achieve >1000 HIV-RNA copies/mL and the proportion of participants off ART was observed, being higher compared to historical controls. Just before ATI, α4β7 expression was associated with HIV-1 DNA and RNA in peripheral blood and with PD1 and TIGIT levels. Importantly, a complete blocking of α4β7 was observed on peripheral CD4+ T-cells but not in gut (ileum and caecum), where α4β7 blockade and vedolizumab levels were inversely associated with HIV-1 DNA. Our findings support α4β7 as an important determinant in HIV-1 reservoir size, suggesting the complete α4β7 blockade in tissue as a promising tool for HIV-cure combination strategies.
Authors
Maria Reyes Jimenez-Leon, Carmen Gasca-Capote, Cristina Roca-Oporto, Nuria Espinosa, Salvador Sobrino, Maria Fontillon-Alberdi, Ce Gao, Isabelle Roseto, Gregory Gladkov, Inmaculada Rivas-Jeremias, Karin Neukam, Jose German Sanchez-Hernandez, Raul Rigo-Bonnin, Antonio J. Cervera-Barajas, Rosario Mesones, Federico García, Ana Isabel Alvarez-Rios, Sara Bachiller, Joana Vitalle, Alberto Perez-Gomez, María Inés Camacho-Sojo, Isabel Gallego, Christian Brander, Ian McGowan, Beatriz Mothe, Pompeyo Viciana, Xu Yu, Mathias Lichterfeld, Luis F. Lopez-Cortes, Ezequiel Ruiz-Mateos
Citation Information: JCI Insight. 2024;9(13):e173215. https://doi.org/10.1172/jci.insight.173215.
Abstract
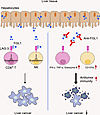
Fibrinogen-like protein 1 (FGL1) contributes to the proliferation and metabolism of hepatocytes; however, as a major ligand of the immune checkpoint, its role in the liver regional immune microenvironment is poorly understood. Hepatocytes specifically and highly expressed FGL1 under normal physiological conditions. Increases in hepatic CD8+ T and NK cell numbers and functions were found in Fgl1-deficient (Fgl1–/–) mice, but not in the spleen or lymph node, similar to findings in anti-FGL1 mAb–treated wild-type mice. Furthermore, Fgl1 deficiency or anti-FGL1 mAb blockade restrained liver metastasis and slowed the growth of orthotopic tumors, with significantly prolonged survival of tumor-bearing mice. Tumor-infiltrating hepatic CD8+ T and NK cells upregulated the expression of lymphocyte activation gene-3 (LAG-3) and exhibited stronger antitumor activities after anti-FGL1 treatment. The antitumor efficacy of FGL1 blockade depended on cytotoxic T lymphocytes and NK cells, demonstrated by using a cell-deficient mouse model and cell transfer in vivo. In vitro, FGL1 directly inhibited hepatic T and NK cells related to the receptor LAG-3. In conclusion, hepatocyte-derived FGL1 played critical immunoregulatory roles in the liver and contributed to liver metastasis and tumor growth by inhibiting CD8+ T and NK cell functions via the receptor LAG-3, providing a new strategy for liver cancer immunotherapy.
Authors
Fengjia Xi, Haoyu Sun, Hui Peng, Zhexiong Lian, Haiming Wei, Zhigang Tian, Rui Sun, Yongyan Chen
Citation Information: JCI Insight. 2024;9(13):e171830. https://doi.org/10.1172/jci.insight.171830.
Abstract
Optimization of protective immune responses against SARS-CoV-2 remains an urgent worldwide priority. In this regard, type III IFN (IFN-λ) restricts SARS-CoV-2 infection in vitro, and treatment with IFN-λ limits infection, inflammation, and pathogenesis in murine models. Furthermore, IFN-λ has been developed for clinical use to limit COVID-19 severity. However, whether endogenous IFN-λ signaling has an effect on SARS-CoV-2 antiviral immunity and long-term immune protection in vivo is unknown. In this study, we identified a requirement for IFN-λ signaling in promoting viral clearance and protective immune programming in SARS-CoV-2 infection of mice. Expression of both IFN and IFN-stimulated gene (ISG) in the lungs were minimally affected by the absence of IFN-λ signaling and correlated with transient increases in viral titers. We found that IFN-λ supported the generation of protective CD8 T cell responses against SARS-CoV-2 by facilitating accumulation of CD103+ DC in lung draining lymph nodes (dLN). IFN-λ signaling specifically in DCs promoted the upregulation of costimulatory molecules and the proliferation of CD8 T cells. Intriguingly, antigen-specific CD8 T cell immunity to SARS-CoV-2 was independent of type I IFN signaling, revealing a nonredundant function of IFN-λ. Overall, these studies demonstrate a critical role for IFN-λ in protective innate and adaptive immunity upon infection with SARS-CoV-2 and suggest that IFN-λ serves as an immune adjuvant to support CD8 T cell immunity.
Authors
Abigail D. Solstad, Parker J. Denz, Adam D. Kenney, Najmus S. Mahfooz, Samuel Speaks, Qiaoke Gong, Richard T. Robinson, Matthew E. Long, Adriana Forero, Jacob S. Yount, Emily A. Hemann
Citation Information: JCI Insight. 2024;9(13):e178216. https://doi.org/10.1172/jci.insight.178216.
Abstract
Staphylococcus aureus is a major human pathogen. An effective anti–S. aureus vaccine remains elusive as the correlates of protection are ill-defined. Targeting specific T cell populations is an important strategy for improving anti–S. aureus vaccine efficacy. Potential bottlenecks that remain are S. aureus–induced immunosuppression and the impact this might have on vaccine-induced immunity. S. aureus induces IL-10, which impedes effector T cell responses, facilitating persistence during both colonization and infection. Thus, it was hypothesized that transient targeting of IL-10 might represent an innovative way to improve vaccine efficacy. In this study, IL-10 expression was elevated in the nares of persistent carriers of S. aureus, and this was associated with reduced systemic S. aureus–specific Th1 responses. This suggests that systemic responses are remodeled because of commensal exposure to S. aureus, which negatively implicates vaccine function. To provide proof of concept that targeting immunosuppressive responses during immunization may be a useful approach to improve vaccine efficacy, we immunized mice with T cell–activating vaccines in combination with IL-10–neutralizing antibodies. Blocking IL-10 during vaccination enhanced effector T cell responses and improved bacterial clearance during subsequent systemic and subcutaneous infection. Taken together, these results reveal a potentially novel strategy for improving anti–S. aureus vaccine efficacy.
Authors
Alanna M. Kelly, Karen N. McCarthy, Tracey J. Claxton, Simon R. Carlile, Eoin C. O’Brien, Emilio G. Vozza, Kingston H.G. Mills, Rachel M. McLoughlin
Citation Information: JCI Insight. 2024. https://doi.org/10.1172/jci.insight.177555.
Abstract
Solid organ transplantation remains the life-saving treatment for end-stage organ failure, but chronic rejection remains a major obstacle to long-term allograft outcomes and has not improved substantially. Tertiary lymphoid organs (TLO) are ectopic lymphoid structures that form under conditions of chronic inflammation, and evidence from human transplantation suggests that TLO regularly form in allografts undergoing chronic rejection. In this study, we utilized a mouse renal transplantation model and manipulation of the lymphotoxin alpha (LTα) – lymphotoxin beta receptor (LTβR) pathway, which is essential for TLO formation, to define the role of TLO in transplantation. We showed that intragraft TLO are sufficient to activate the alloimmune response and mediate graft rejection in a model where the only lymphoid organs are TLO in the allograft. When transplanted to recipients with a normal set of secondary lymphoid organs, the presence of graft TLO or LTα overexpression accelerated rejection. If the LTβR pathway was disrupted in the donor graft, TLO formation was abrogated, and graft survival prolonged. Intravital microscopy of renal TLO demonstrated that local T and B cell activation in TLOs is similar to that observed in secondary lymphoid organs. In summary, we demonstrated that immune activation in TLO contributes to local immune responses, leading to earlier allograft failure. TLO and the LTαβ-LTβR pathway are therefore prime targets to limit local immune responses and prevent allograft rejection. These findings are applicable to other diseases such as autoimmunity or tumors, where either limiting or boosting local immune responses is beneficial and improves disease outcomes.
Authors
Gang Zhang, Neda Feizi, Daqiang Zhao, Latha Halesha, Amanda L. Williams, Parmjeet S. Randhawa, Khodor I. Abou-Daya, Martin H. Oberbarnscheidt
Citation Information: JCI Insight. 2024. https://doi.org/10.1172/jci.insight.171605.
Abstract
Upon infection, naïve CD8+ T cells differentiate into cytotoxic effector cells to eliminate the pathogen-infected cells. Although many mechanisms underlying this process have been demonstrated, the regulatory role of chromatin remodel system in this process remains largely unknown. Here we showed that BRD7, a component of the polybromo-associated BRG1-associated factor complex (PBAF), was required for naïve CD8+ T cells to differentiate into functional short-lived effector cells (SLECs) in response to acute infections caused by influenza virus or lymphocytic choriomeningitis virus (LCMV). BRD7-deficiency in CD8+ T cells resulted in profound defects in effector population and functions, thereby impairing viral clearance and host recovery. Further mechanical studies indicated that the expression of BRD7 significantly turned to high from naïve CD8+ T cells to effector cells, bridged BRG1 and PBRM1 to the core module of PBAF complex, consequently facilitating the assembly of PBAF complex rather than BAF complex in the effector cells. The PBAF complex changed the chromatin accessibility at the loci of Tbx21 gene and up-regulated its expression, leading to the maturation of effector T cells. Our research confirms BRD7 and the PBAF complex are key in CD8+ T cell development and present a significant target for advancing immune therapies.
Authors
Feng Huang, Yingtong Lin, Yidan Qiao, Yaochang Yuan, Zhihan Zhong, Baohong Luo, Yating Wu, Jun Liu, Jingliang Chen, Wanying Zhang, Hui Zhang, Bingfeng Liu
Citation Information: JCI Insight. 2024. https://doi.org/10.1172/jci.insight.167967.
Abstract
Beside suppressing immune responses, regulatory T cells (Tregs) maintain tissue homeostasis and control systemic metabolism. Whether iron is involved in Treg-mediated tolerance is completely unknown. Here, we showed that the transferrin receptor CD71 was upregulated on activated Tregs infiltrating human liver cancer. Mice with a Treg-restricted CD71 deficiency spontaneously developed a scurfy-like disease, caused by impaired perinatal Treg expansion. CD71-null Tregs displayed decreased proliferation and tissue-Treg signature loss. In perinatal life, CD71 deficiency in Tregs triggered hepatic iron overload response, characterized by increased hepcidin transcription and iron accumulation in macrophages. Lower bacterial diversity, and reduction of beneficial species, were detected in the fecal microbiota of CD71 conditional knock-out neonates. Our findings indicate that CD71-mediated iron absorption is required for Treg perinatal expansion and related to systemic iron homeostasis and bacterial gut colonization. Therefore, we hypothesize that Tregs establish nutritional tolerance through competition for iron during bacterial colonization after birth.
Authors
Ilenia Pacella, Alessandra Pinzon Grimaldos, Alessandra Rossi, Gloria Tucci, Marta Zagaglioni, Elena Potenza, Valeria Pinna, Ivano Rotella, Ilenia Cammarata, Valeria Cancila, Beatrice Belmonte, Claudio Tripodo, Giuseppe Pietropaolo, Chiara Di Censo, Giuseppe Sciumè, Valerio Licursi, Giovanna Peruzzi, Ylenia Antonucci, Silvia Campello, Francesca Guerrieri, Valerio Iebba, Rita Prota, Maria Di Chiara, Gianluca Terrin, Valerio De Peppo, Gian Luca Grazi, Vincenzo Barnaba, Silvia Piconese
Citation Information: JCI Insight. 2024. https://doi.org/10.1172/jci.insight.178499.
Abstract
Rheumatoid arthritis (RA) management lean toward achieving remission or low-disease activity. In this study, we conducted single-cell RNA sequencing (scRNAseq) of peripheral blood mononuclear cells (PBMCs) from 36 individuals (18 RA patients and 18 matched controls, accounting for age, sex, race, and ethnicity), to identify disease-relevant cell subsets and cell type-specific signatures associated with disease activity. Our analysis revealed 18 distinct PBMC subsets, including an IFITM3 overexpressing Interferon-activated (IFN-activated) monocyte subset. We observed an increase in CD4+ T effector memory cells in patients with moderate to high disease activity (DAS28-CRP ≥ 3.2), and a decrease in non-classical monocytes in patients with low disease activity or remission (DAS28-CRP < 3.2). Pseudobulk analysis by cell type identified 168 differentially expressed genes between RA and matched controls, with a downregulation of pro-inflammatory genes in the gamma-delta T cells subset, alteration of genes associated with RA predisposition in the IFN-activated subset, and non-classical monocytes. Additionally, we identified a gene signature associated with moderate-high disease activity, characterized by upregulation of pro-inflammatory genes such as TNF, JUN, EGR1, IFIT2, MAFB, G0S2, and downregulation of genes including HLA-DQB1, HLA-DRB5, TNFSF13B. Notably, cell-cell communication analysis revealed an upregulation of signaling pathways, including VISTA, in both moderate-high and remission-low disease activity contexts. Our findings provide valuable insights into the systemic cellular and molecular mechanisms underlying RA disease activity.
Authors
Marie Binvignat, Brenda Y. Miao, Camilla Wibrand, Monica M. Yang, Dmitry Rychkov, Emily Flynn, Joanne Nititham, Whitney Tamaki, Umair Khan, Alexander Carvidi, Melissa Krueger, Erene C. Niemi, Yang Sun, Gabriela K. Fragiadakis, Jérémie Sellam, Encarnita Mariotti-Ferrandiz, David Klatzmann, Andrew J. Gross, Chun Jimmie Ye, Atul J. Butte, Lindsey A. Criswell, Mary C. Nakamura, Marina Sirota
Citation Information: JCI Insight. 2024;9(12):e172959. https://doi.org/10.1172/jci.insight.172959.
Abstract
Plasmacytoid dendritic cells (pDCs) are first responders to tissue injury, where they prime naive T cells. The role of pDCs in physiologic wound repair has been examined, but little is known about pDCs in diabetic wound tissue and their interactions with naive CD4+ T cells. Diabetic wounds are characterized by increased levels of inflammatory IL-17A cytokine, partly due to increased Th17 CD4+ cells. This increased IL-17A cytokine, in excess, impairs tissue repair. Here, using human tissue and murine wound healing models, we found that diabetic wound pDCs produced excess IL-6 and TGF-β and that these cytokines skewed naive CD4+ T cells toward a Th17 inflammatory phenotype following cutaneous injury. Further, we identified that increased IL-6 cytokine production by diabetic wound pDCs is regulated by a histone demethylase, Jumonji AT-rich interactive domain 1C histone demethylase (JARID1C). Decreased JARID1C increased IL-6 transcription in diabetic pDCs, and this process was regulated upstream by an IFN-I/TYK2/JAK1,3 signaling pathway. When inhibited in nondiabetic wound pDCs, JARID1C skewed naive CD4+ T cells toward a Th17 phenotype and increased IL-17A production. Together, this suggests that diabetic wound pDCs are epigenetically altered to increase IL-6 expression that then affects T cell phenotype. These findings identify a therapeutically manipulable pathway in diabetic wounds.
Authors
Christopher O. Audu, Sonya J. Wolf, Amrita D. Joshi, Jadie Y. Moon, William J. Melvin, Sriganesh B. Sharma, Frank M. Davis, Andrea T. Obi, Rachel Wasikowski, Lam C. Tsoi, Emily C. Barrett, Kevin D. Mangum, Tyler M. Bauer, Steven L. Kunkel, Beth B. Moore, Katherine A. Gallagher
No posts were found with this tag.