Journal Description
Reproductive Medicine
Reproductive Medicine
is an international, peer-reviewed, open access journal on obstetrics and gynecology published quarterly online by MDPI.
- Open Access— free for readers, with article processing charges (APC) paid by authors or their institutions.
- High Visibility: indexed within ESCI (Web of Science), FSTA, and other databases.
- Rapid Publication: manuscripts are peer-reviewed and a first decision is provided to authors approximately 41.2 days after submission; acceptance to publication is undertaken in 5.4 days (median values for papers published in this journal in the first half of 2024).
- Recognition of Reviewers: APC discount vouchers, optional signed peer review, and reviewer names published annually in the journal.
Impact Factor:
1.1 (2023);
5-Year Impact Factor:
1.0 (2023)
Latest Articles
Temporal Evaluation of a Minimally Invasive Method of Preimplantation Genetic Testing for Aneuploidy (mi-PGT-A) in Human Embryos
Reprod. Med. 2024, 5(3), 97-112; https://doi.org/10.3390/reprodmed5030011 (registering DOI) - 8 Jul 2024
Abstract
►
Show Figures
Preimplantation genetic testing for aneuploidy (PGT-A) has become a useful approach for embryo selection following IVF and ICSI. However, the biopsy process associated with PGT-A is expensive, prone to errors in embryo ploidy determination, and potentially damaging, impacting competence and implantation potential. Therefore,
[...] Read more.
Preimplantation genetic testing for aneuploidy (PGT-A) has become a useful approach for embryo selection following IVF and ICSI. However, the biopsy process associated with PGT-A is expensive, prone to errors in embryo ploidy determination, and potentially damaging, impacting competence and implantation potential. Therefore, a less invasive method of PGT-A would be desirable and more cost-effective. Noninvasive methods for PGT-A (ni-PGT-A) have been well-studied but present limitations in terms of cf-DNA origin and diagnostic accuracy. Minimally invasive pre-implantation genetic testing (mi-PGT-A) for frozen-thawed embryo transfer is a promising, less studied approach that utilizes a combination of spent culture media (SCM) and blastocoelic fluid (BF)-derived cell-free (CF)-DNA for genetic testing. This study aimed to optimize the effectiveness of mi-PGT-A for aneuploidy diagnosis by investigating the optimal temporal sequence for this protocol. SCM+BF was collected at either 48 or 72 h of culture after thawing day 3 preimplantation embryos. cf-DNA in the SCM+BF was amplified, analyzed by next-generation sequencing (NGS) and compared with results from the corresponding whole embryos (WEs) obtained from human embryos donated for research. Fifty-three (42 expanded blastocysts, 9 early blastocysts, and 2 morula) WE and SCM+BF samples were analyzed and compared. The overall concordance rate between SCM+BF and WE was 60%. Gender and ploidy concordance improved with extended culture time from 48 h (73% and 45%) to 72 h (100% and 64%), respectively. These results demonstrate that SCM+BF-derived cf-DNA can be successfully used for mi-PGT-A. Our findings indicate that longer embryo culture time prior to SCM+BF-derived cf-DNA analysis improves DNA detection rate and concordance with WEs and decreases the proportion of false positive results.
Full article
Open AccessCommunication
Prevalence of Pathogenic Microbes within the Endometrium in Normal Weight vs. Obese Women with Infertility
by
Sarah King, Florence Osei and Courtney Marsh
Reprod. Med. 2024, 5(2), 90-96; https://doi.org/10.3390/reprodmed5020010 - 6 Jun 2024
Abstract
►▼
Show Figures
This study investigates the association between body mass index (BMI) and the composition of the endometrial microbiota in infertile women of childbearing age. This is a retrospective clinical study comparing the endometrial microbiota across body weight in 132 patients presenting for care at
[...] Read more.
This study investigates the association between body mass index (BMI) and the composition of the endometrial microbiota in infertile women of childbearing age. This is a retrospective clinical study comparing the endometrial microbiota across body weight in 132 patients presenting for care at an infertility clinic. The reason for infertility was recurrent pregnancy loss (RPL) or implantation failure with a prior IVF cycle. Microbe analysis was completed by Igenomix Laboratory (Valencia, Spain) using two comprehensive panels. Patients were separated into three groups based on their results: normal, dysbiotic, and pathogenic. Prevalence of these groups was compared across BMI categories and statistical analysis was used to determine significance. Of the 132 endometrial samples collected, 80 (60.6%) were normal, 16 (12.1%) were dysbiotic, and 36 (27.3%) were pathogenic. Patients with a BMI ≥ 30 showed a statistically significant increase in pathogenic endometrium compared to normal weight controls (p = 0.029). Our conclusion is that the prevalence of pathogenic endometrium was significantly higher in the obese group compared with normal weight controls. There is a possible association between obesity and the endometrial microbiome.
Full article

Figure 1
Open AccessCommunication
A Comparison of the Frequency of Trisomy 13, 18, and 21 Using Non-Invasive Prenatal Testing According to Diminished vs. Normal Egg Reserve and Age
by
Brooke Neumann, Nicole Weitz, Jerome H. Check, Carrie Wilson, Ann Diantonio and Megan O’Neil
Reprod. Med. 2024, 5(2), 81-89; https://doi.org/10.3390/reprodmed5020009 - 4 Jun 2024
Abstract
Background: This study’s aim was to determine whether diminished oocyte reserve (DOR) increases the risk of having a fetus with trisomy 13, 18, or 21 at 10 weeks as evaluated by non-invasive prenatal testing (NIPT) and to evaluate the confounding effect of advanced
[...] Read more.
Background: This study’s aim was to determine whether diminished oocyte reserve (DOR) increases the risk of having a fetus with trisomy 13, 18, or 21 at 10 weeks as evaluated by non-invasive prenatal testing (NIPT) and to evaluate the confounding effect of advanced age. Methods: NIPT was undertaken in all pregnancies conceived through natural treatment or assisted reproductive technology that reached 10 weeks from conception with a viable fetus from one infertility center. Data were stratified according to serum anti-Mullerian hormone (AMH) < 1 ng/mL and ≥1 ng/mL. Results: No woman < 39 or with AMH ≥ 1 ng/mL showed trisomy 13, 18, or 21 by NIPT. Only women ≥ age 39 with DOR had one of these trisomies. Conclusions: Hopefully these data, coupled with other factors, e.g., etiology of infertility, age, insurance, or financial circumstances, and personal views of pregnancy termination, will aid patients with DOR when choosing treatment options, including natural conception, IVF-ET, IVF with pre-implantation genetic testing for aneuploidy, or transfer of fertilized donor eggs.
Full article
Open AccessArticle
Kinetic Energy and the Free Energy Principle in the Birth of Human Life
by
Yasunari Miyagi, Yasuyuki Mio, Keitaro Yumoto, Rei Hirata, Toshihiro Habara and Nobuyoshi Hayashi
Reprod. Med. 2024, 5(2), 65-80; https://doi.org/10.3390/reprodmed5020008 - 21 May 2024
Abstract
►▼
Show Figures
The retrospective noninterventional study investigated the kinetic energy of video images of 18 fertilized eggs (7 were normal and 11 were abnormal) recorded by a time-lapse device leading up to the beginning of the first cleavage. The norm values of cytoplasmic particles were
[...] Read more.
The retrospective noninterventional study investigated the kinetic energy of video images of 18 fertilized eggs (7 were normal and 11 were abnormal) recorded by a time-lapse device leading up to the beginning of the first cleavage. The norm values of cytoplasmic particles were measured by the optical flow method. Three phase profiles for normal cases were found regarding the kinetic energy: 2.199 × 10−24 ± 2.076 × 10−24, 2.369 × 10−24 ± 1.255 × 10−24, and 1.078 × 10−24 ± 4.720 × 10−25 (J) for phases 1, 2, and 3, respectively. In phase 2, the energies were 2.369 × 10−24 ± 1.255 × 10−24 and 4.694 × 10−24 ± 2.996 × 10−24 (J) (mean ± SD, p = 0.0372), and the time required was 8.114 ± 2.937 and 6.018 ± 5.685 (H) (p = 0.0413) for the normal and abnormal cases, respectively. The kinetic energy change was considered a condition for applying the free energy principle, which states that for any self-organized system to be in equilibrium in its environment, it must minimize its informational free energy. The kinetic energy, while interpreting it in terms of the free energy principle suggesting clinical usefulness, would further our understanding of the phenomenon of fertilized egg development with respect to the birth of human life.
Full article

Figure 1
Open AccessCommunication
Risk of Obstetric Anal Sphincter Injury by Delivering Provider
by
Taniya V. Walker, Ciara Bryson, Sara Rahman and Charelle M. Carter-Brooks
Reprod. Med. 2024, 5(2), 57-64; https://doi.org/10.3390/reprodmed5020007 - 8 May 2024
Abstract
Introduction and Hypothesis: Obstetric anal sphincter injuries (OASIs) complicate 5.8% of vaginal deliveries. Our objective was to assess if the primary delivery provider, a nurse-midwife versus physician obstetrician, is associated with OASIs. Methods: We performed a secondary analysis of the Consortium of Safe
[...] Read more.
Introduction and Hypothesis: Obstetric anal sphincter injuries (OASIs) complicate 5.8% of vaginal deliveries. Our objective was to assess if the primary delivery provider, a nurse-midwife versus physician obstetrician, is associated with OASIs. Methods: We performed a secondary analysis of the Consortium of Safe Labor, a multicenter, retrospective cohort study. Included were nulliparous women with singleton, vaginal delivery at ≥37 weeks from 2002 to 2008. Women were excluded if delivery was complicated by shoulder dystocia or from sites without midwife deliveries. Student’s t-tests, chi-squared analysis, and Fisher’s exact test were used as appropriate. Multivariable logistic regression and propensity score-matching analyses were performed. Results: Of 228,668 births at 19 sites, 2735 births from 3 sites met the inclusion criteria: 1551 physician and 1184 midwife births. Of all births, 4.2% (n = 116) were complicated by OASIs. Physician patients were older, more often White, privately insured, with higher BMI, more medical co-morbidities, and labor inductions/augmentations. Midwife patients had higher fetal gestational age and infant birth weights (all p < 0.05). OASIs were more common in physician compared to midwife births (5.9% vs. 2.0%, p < 0.0001). This difference persisted in multivariable logistic regression. OASIs were 2.4 (95%CI 1.5–3.9) times more likely with physician delivery when controlling for maternal heart disease, episiotomy, increasing maternal age, decreasing maternal BMI, non-White race, and increasing birthweight. The AUC was 0.78. With propensity score matching, OASI rates remained higher amongst physician births (6.6% vs. 1.8%, p < 0.0001; aOR 3.8 (95%CI 2.0–7.1)). Conclusion: OASIs were more common in physician compared to midwife deliveries even when controlling for other associated factors.
Full article
Open AccessArticle
IL17A Suppresses IGFBP1 in Human Endometrial Stromal Cells
by
Susumu Tanaka, Misa Sawachika, Namika Yoshida, Kensuke Futani, Hiromi Murata and Hidetaka Okada
Reprod. Med. 2024, 5(2), 43-56; https://doi.org/10.3390/reprodmed5020006 - 26 Apr 2024
Abstract
►▼
Show Figures
Interleukin (IL) 17A has been implicated in preeclampsia, preterm labor, and miscarriage. IL17A production in non-lymphoid tissues is mainly carried out by unconventional γδ17T cells. Innate lymphoid cells (ILCs) 3, a subgroup of innate lymphocytes, can also be a source of IL17A in
[...] Read more.
Interleukin (IL) 17A has been implicated in preeclampsia, preterm labor, and miscarriage. IL17A production in non-lymphoid tissues is mainly carried out by unconventional γδ17T cells. Innate lymphoid cells (ILCs) 3, a subgroup of innate lymphocytes, can also be a source of IL17A in the endometrium and are required from implantation to early pregnancy, with their regulation ensuring that pregnancy continues. Herein, we examined the expression of γδ17T cells and ILC3 regulators IL1B, IL23A, and IL17D and IL17A receptors (IL17RA/IL17RC) in human endometrial stromal cells (EnSCs) and cell lines (KC02-44D). Accordingly, quantitative polymerase chain reaction and immunoblotting were employed. IL1B, IL23A, and IL17D were significantly upregulated in decidualized EnSCs and KC02-44D cells. A significant augmentation in IL17RA/IL17RC was also observed in decidualization. IL17A stimulation of KC02-44D cells during decidualization suppressed the decidualization marker IGFBP1. The involvement of transcription factor Forkhead box protein O1 (FOXO1) in this repression was reflected by its translocation from the nucleus into the cytoplasm. A role for IkB kinase alpha in FOXO1 phosphorylation-mediated migration was also suggested. Taken together, our findings indicate that the secretion of IL17A by γδ17T and ILC3 cells in the uterus contributes to EnSCs function and may play critical roles in regulating IGFBP1-mediated implantation and fetal growth.
Full article
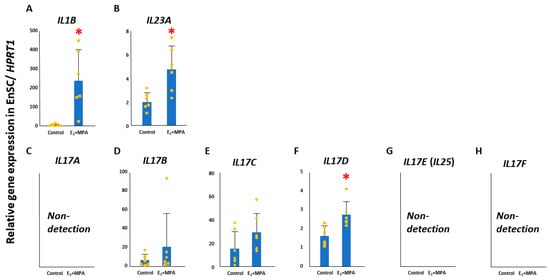
Figure 1
Open AccessArticle
Defining the Limits of Postpartum Leukocytosis: A Retrospective Cohort Study
by
Lindsay A. Hartup, Elizabeth Guarisco, Xuemei Song, Zhu Wang and Angela R. Boyd
Reprod. Med. 2024, 5(2), 33-42; https://doi.org/10.3390/reprodmed5020005 - 25 Apr 2024
Abstract
►▼
Show Figures
There are established reference ranges for many laboratory values during pregnancy. Fewer studies exist regarding the expected white blood cell (WBC) count after delivery. The aim of this study was to determine appropriate postpartum leukocytosis in a diverse patient cohort. Patients who delivered
[...] Read more.
There are established reference ranges for many laboratory values during pregnancy. Fewer studies exist regarding the expected white blood cell (WBC) count after delivery. The aim of this study was to determine appropriate postpartum leukocytosis in a diverse patient cohort. Patients who delivered a live fetus at 37 weeks or later were retrospectively identified. Complete blood counts collected on hospital admission and postpartum day one were used to quantify the change in WBC count associated with delivery. A total of 2245 patients were included; of these patients, 1476 delivered vaginally and 769 delivered via cesarean section. The average change in WBC count was 2.99 × 103/mm3. A WBC count of 20.19 × 103/mm3 defined the 95th percentile. The average rise in WBC count was 3.31 × 103/mm3 after vaginal delivery and 2.34 × 103/mm3 after cesarean section (p < 0.001). Patients with chorioamnionitis or endometritis had an average postpartum WBC rise of 7.38 × 103/mm3 compared to 2.99 × 103/mm3 in controls (p < 0.001). There was no difference in WBC count rise with comorbid asthma, diabetes, or chronic hypertension. A greater WBC count rise was found in patients with pregnancy-induced hypertension. This study provides reference values for the average rise in WBC count after delivery and the 95th percentile postpartum WBC count in a diverse, medically complex patient population with and without delivery complications. Our findings further highlight maternal medical comorbidities that may contribute to the degree of postpartum leukocytosis.
Full article
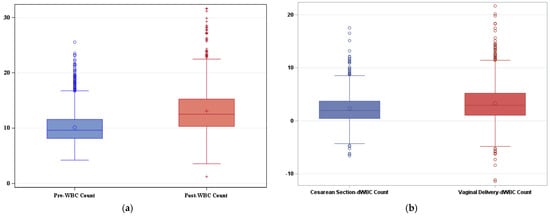
Figure 1
Open AccessCorrection
Correction: Rose et al. The Effect of In Vitro Maturation (IVM) Protocol Changes on Measures of Oocyte/Embryo Competence. Reprod. Med. 2023, 4, 65–73
by
Bruce I. Rose, Kevin Nguyen and Samuel E. Brown
Reprod. Med. 2024, 5(2), 32; https://doi.org/10.3390/reprodmed5020004 - 12 Apr 2024
Abstract
**Samuel E [...]
Full article
Open AccessArticle
Pre-Operative Anxiety Related to Major Urogynecologic Surgery: Insights from Perioperative Survey Data in Maine
by
Nadi Nina Kaonga, Yanghee Courbron, Emmy Holmgren, Eliot Konzal, Whitney Williams, Mary Brandes and Caroline Foust-Wright
Reprod. Med. 2024, 5(1), 23-31; https://doi.org/10.3390/reprodmed5010003 - 7 Mar 2024
Abstract
►▼
Show Figures
Background: Higher levels of pre-operative anxiety are associated with adverse outcomes according to the cardiothoracic and orthopedic literature on emergent surgeries. There are limited data on pre-operative anxiety levels in the gynecologic setting. This study sought to identify predictive variables for high pre-operative
[...] Read more.
Background: Higher levels of pre-operative anxiety are associated with adverse outcomes according to the cardiothoracic and orthopedic literature on emergent surgeries. There are limited data on pre-operative anxiety levels in the gynecologic setting. This study sought to identify predictive variables for high pre-operative anxiety levels in patients undergoing major urogynecologic surgery. Methods: Pre- and post-operative surveys that included demographic data, a modification of the Amsterdam Pre-Operative Anxiety and Information Scale, and open-ended questions regarding anxiety were administered. Descriptive, univariate and multivariate analyses were used to analyze the quantitative elements of the survey data. The qualitative components of the survey data were coded and analyzed using thematic analyses. Results: A total of 54 participants completed the pre-operative survey. The median age was 62 years old, and the majority were employed (n = 34, 60.7%). Roughly 1/3 had been diagnosed with a mental health condition (n = 19, 33.9%) and nearly all had other health conditions (n = 51, 91%). The baseline APAIS score ranged from 9 to 40, with higher scores reflecting higher levels of pre-operative anxiety. The median APAIS score was 24, with a score equal to or greater than 30 being in the highest tertile. Conclusion: No associations were made between the variables and pre-operative anxiety levels. However, useful insights into our patient population were made.
Full article
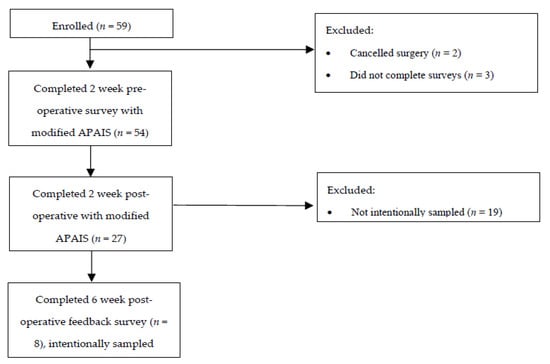
Figure 1
Open AccessArticle
Diabetes Technology in Pregnant Women with Type 1 Diabetes—Distribution and Effects on Glycemic Regulation and Perinatal Outcomes
by
Sara Yalda Ghaur, Pernille Bundgaard Grinderslev, Magnus Leth-Møller, Per Glud Ovesen, Jens Fuglsang, Sanne Fisker, H. David McIntyre and Ulla Kampmann
Reprod. Med. 2024, 5(1), 12-22; https://doi.org/10.3390/reprodmed5010002 - 7 Feb 2024
Abstract
►▼
Show Figures
Pregnancies complicated by type 1 diabetes (TID) are associated with an increased risk of obstetric and neonatal adverse outcomes. Optimal glycemic control prior to and through pregnancy is crucial to reduce complications. The use of diabetes technology is rapidly increasing. The aim of
[...] Read more.
Pregnancies complicated by type 1 diabetes (TID) are associated with an increased risk of obstetric and neonatal adverse outcomes. Optimal glycemic control prior to and through pregnancy is crucial to reduce complications. The use of diabetes technology is rapidly increasing. The aim of the study was to investigate the use and effects of diabetes technology in pregnant women with type 1 diabetes. A retrospective cohort study was conducted; 84 women were included in the analysis and were divided into subgroups according to their glucose monitoring method and insulin delivery method. HbA1c values declined during pregnancy in all subgroups with no significant difference between the subgroups. A difference was, however, found in birth weight z-scores. Women using a sensor and an insulin pump had larger babies compared to women without these treatment modalities. The results of the study indicate that diabetes technology, including insulin pumps and/or glucose sensors are not superior to self-monitoring blood glucose measurement and multiple daily injection insulin therapy, which is comforting in the light of the unequal access to health benefits.
Full article

Graphical abstract
Open AccessArticle
Antenatal Secondhand Smoke (SHS) Exposure and the Receptor for Advanced Glycation End-Products (RAGE)
by
Katrina L. Curtis, Kelsey M. Hirshi, Kary Tsai, Evan T. Clark, Brendan M. Stapley, Benjamin T. Bikman, Paul R. Reynolds and Juan Arroyo
Reprod. Med. 2024, 5(1), 1-11; https://doi.org/10.3390/reprodmed5010001 - 30 Jan 2024
Abstract
►▼
Show Figures
Exposure to secondhand smoke (SHS) during fetal development results in negative postnatal effects, including altered organ development, changes in metabolism, and increased risk of respiratory illness. Previously, we found the induction of intrauterine growth restriction (IUGR) dependent on the expression of the receptor
[...] Read more.
Exposure to secondhand smoke (SHS) during fetal development results in negative postnatal effects, including altered organ development, changes in metabolism, and increased risk of respiratory illness. Previously, we found the induction of intrauterine growth restriction (IUGR) dependent on the expression of the receptor for advanced glycation end-products (RAGE) in mice treated with SHS. Furthermore, antenatal SHS exposure increases RAGE expression in the fetal lung. Our objective was to determine the postnatal effects of antenatal SHS treatment in 4- and 12-week-old offspring. Pregnant animals were treated with SHS via a nose-only delivery system (Scireq Scientific, Montreal, Canada) for 4 days (embryonic day 14.5 through 18.5), and offspring were evaluated at 4 or 12 weeks of age. Animal and organ weights were measured, and lungs were histologically characterized. Blood pressure and heart rates were obtained, and RAGE protein expression was determined in the lungs of control and treated animals. We observed the following: (1) significant decreases in animal, liver, and heart weights at 4 weeks of age; (2) increased blood pressure in 4-week-old animals; and (3) increased RAGE expression in the lungs of the 4-week-old animals. Our results suggest an improvement in these metrics by 12 weeks postnatally such that measures were not different regardless of RA or SHS exposure. Increased RAGE expression in lungs from 4-week-old mice antenatally treated with SHS suggests a possible role for this important smoke-mediated receptor in establishing adult disease following IUGR pregnancies.
Full article
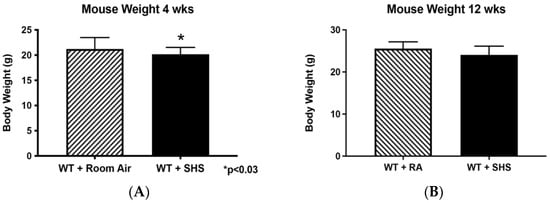
Figure 1
Open AccessArticle
Exposure of Early Postnatal Oocytes to Chemotherapy Alters the Potential Ovarian Reserve, According to an Ex Vivo Mouse Model
by
Meghan C. H. Ozcan, Julienne Chaqour, Morgan F. Woodman-Sousa and Kathryn J. Grive
Reprod. Med. 2023, 4(4), 248-258; https://doi.org/10.3390/reprodmed4040023 - 18 Dec 2023
Abstract
►▼
Show Figures
Current safety data on chemotherapy during pregnancy are based on studies which focus on the mother and do not explore reproductive health and fecundity potential within the exposed offspring. We designed this randomized ex vivo animal study to evaluate the effect of chemotherapy
[...] Read more.
Current safety data on chemotherapy during pregnancy are based on studies which focus on the mother and do not explore reproductive health and fecundity potential within the exposed offspring. We designed this randomized ex vivo animal study to evaluate the effect of chemotherapy on the developing ovarian reserve in the exposed offspring. Specimens (100 postnatal day zero C57BL/6 mouse ovaries) were randomized to control or chemotherapy drug exposure and maintained in a hanging well organ culture. Murine ovarian reserve establishment mirrors activity seen in the human fetus but with a significant time shift of the transition to meiotic arrest to the postnatal period. Exposures included: doxorubicin, cyclophosphamide, paclitaxel, docetaxel, and cisplatin. Doxorubicin resulted in a significant loss of 95.2% (p < 0.0001) of oocyte density compared to controls. Cyclophosphamide also caused depletion of 50.5% (p < 0.0001) of oocyte density. Cisplatin, docetaxel, and paclitaxel all demonstrated unique phenotypical changes on the ovaries and their oocytes, without a significant decrease in oocyte density over a five-day exposure. Exposure to chemotherapy may result in profound loss of oogonia during the transition to mature oocytes.
Full article
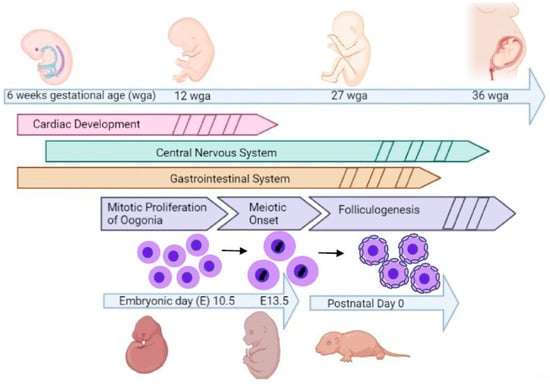
Figure 1
Open AccessCase Report
Prenatal Evaluation of a Fetal Cystic Hygroma: An Unexpected Finding of a De Novo Fetal BRCA1 Deletion Case Report
by
Stephanie C. Laniewski, LauraAnne Hirschler, Anwar M. Iqbal and Neil S. Seligman
Reprod. Med. 2023, 4(4), 242-247; https://doi.org/10.3390/reprodmed4040022 - 23 Oct 2023
Cited by 1
Abstract
This case presents a novel occurrence of a de novo BRCA1 gene deletion in a fetus with a cystic hygroma. Chorionic villus sampling (CVS) was performed for chromosome G-banding analysis, demonstrating a normal karyotype: 46, XX. Chromosome microarray analysis performed as a reflex
[...] Read more.
This case presents a novel occurrence of a de novo BRCA1 gene deletion in a fetus with a cystic hygroma. Chorionic villus sampling (CVS) was performed for chromosome G-banding analysis, demonstrating a normal karyotype: 46, XX. Chromosome microarray analysis performed as a reflex test revealed an 80 kb deletion on 17q21.31, encompassing the BRCA1 gene. Follow-up FISH analysis performed on parental blood samples yielded negative results, confirming that the deletion was de novo in the fetus. Subsequent anatomic ultrasound evaluation showed no identifiable structural defects, and it was concluded that the microdeletion was unlikely to be the cause of the cystic hygroma. Regardless, it will be imperative that the patient’s daughter be appropriately counseled regarding the implications of carrying a BRCA1 deletion and the need for heightened surveillance in adulthood. As BRCA1 genetic testing is traditionally performed on adult patients with informed consent, this case report highlights the need for ongoing conversations and research in the management of incidental fetal diagnosis discovered during routine prenatal testing, as well as the care and counseling of these patients and their families.
Full article
(This article belongs to the Special Issue Feature Papers in Celebration of the Fourth Anniversary of the Founding of Reproductive Medicine)
►▼
Show Figures
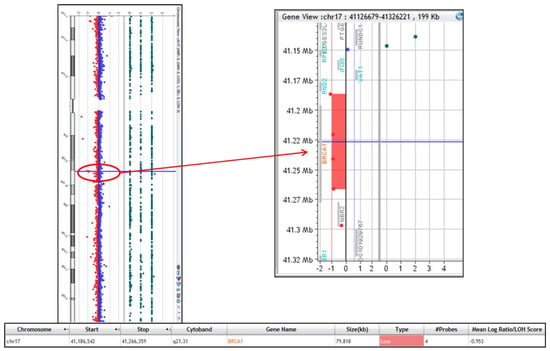
Figure 1
Open AccessArticle
Can We Safely Decrease Early-Term Delivery and Cesarean Section Rate in Pregnancies Complicated by Fetal Transposition of Great Arteries?
by
Angel Chimenea, Lutgardo García-Díaz, Ana Méndez and Guillermo Antiñolo
Reprod. Med. 2023, 4(3), 233-241; https://doi.org/10.3390/reprodmed4030021 - 14 Sep 2023
Abstract
►▼
Show Figures
Background: Transposition of the great arteries (TGA) is a common critical neonatal congenital heart defect. After birth, physiological shunts close rapidly, necessitating early treatment with prostaglandin infusion and balloon-atrial septostomy. Timing of delivery is challenging, balancing the risks and advantages of early-term delivery
[...] Read more.
Background: Transposition of the great arteries (TGA) is a common critical neonatal congenital heart defect. After birth, physiological shunts close rapidly, necessitating early treatment with prostaglandin infusion and balloon-atrial septostomy. Timing of delivery is challenging, balancing the risks and advantages of early-term delivery and specialized care. The aim of this study is to assess the safety of a full-term delivery policy in fetuses diagnosed with TGA. Methods: A retrospective chart review was conducted of 17 women with a prenatal diagnosis of fetal TGA at Virgen del Rocío University Hospital between 2015 and 2021. Primary outcomes included: incidence of preterm, early-term, full-term, and late-term delivery, and rate of cesarean section. Secondary outcomes included: Saturday to Sunday admission and birth, and delivery between 0:00 a.m. and 8:00 a.m. Results: Full-term birth was achieved in 94.1%, reaching a low cesarean delivery rate (17.6%). A total of 82.4% of infants were born on weekdays, and only in three of the cases (17.6%) did delivery occur between 0 a.m. and 8 a.m. The median birth weight was 3300 g. Intravenous prostaglandins were administered in all cases, and 94.1% required balloon-atrial septostomy. Conclusions: In our study favoring full-term delivery, we reduce early-term deliveries and the cesarean section rate in prenatally diagnosed TGA.
Full article
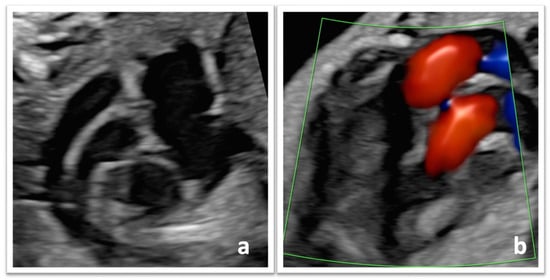
Figure 1
Open AccessReview
Recent Developments in In Vitro Spermatogenesis and Future Directions
by
In Ki Cho and Charles A. Easley
Reprod. Med. 2023, 4(3), 215-232; https://doi.org/10.3390/reprodmed4030020 - 11 Sep 2023
Abstract
Recent developments in stem cell technologies have made significant advancements in the field of in vitro gametogenesis. In vitro gametogenesis (IVG) is a promising technology where functional gametes (sperm or egg cells) can be generated from stem cells. Scientists have made continuous advancements
[...] Read more.
Recent developments in stem cell technologies have made significant advancements in the field of in vitro gametogenesis. In vitro gametogenesis (IVG) is a promising technology where functional gametes (sperm or egg cells) can be generated from stem cells. Scientists have made continuous advancements in the field and successfully derived fully functional sperm from stem cells in mice. Two recent papers generated excitement in IVG by generating bi-maternal and bi-paternal mice from embryonic stem cells (ESCs) and pluripotent stem cells (PSCs). IVG is a promising technology with potential applications that include infertility treatment, fertility preservation, same-sex reproduction, bypassing oocyte depletion in women with advanced age, conservation biology, genetic disorder prevention, and research into human germ cell development. In vitro spermatogenesis (IVS) is the attempt to recreate the process of spermatogenesis in a culture system. Spermatogenesis is essential for male fertility and reproductive health, but it can be impaired by various factors such as genetic defects, environmental toxicants, infections, aging, or medical therapies. Spermatogenesis is a complex and highly regulated process involving multiple cell proliferation, differentiation, and maturation stages. The main challenges of IVS are to provide a suitable microenvironment that mimics the testis in vivo, to support the survival and development of all the cell types involved in spermatogenesis, and to achieve complete and functional spermatogenesis. Therefore, there is a great interest in developing methods to study spermatogenesis in vitro, both for basic research and clinical applications. This review covers recent developments in in vitro spermatogenesis in the past two years. Advances in tissue engineering and regenerative medicine have introduced techniques like ex vivo tissue culture and technologies such as bioreactors, microfluidic systems, and organoids. Bioreactors and microfluidic systems replicate physiological conditions for tissue and cell cultivation, while organoids model organ functionality. Meanwhile, scaffolds, made from various materials, provide essential structural support, guiding the growth and organization of cells into functional tissues.
Full article
(This article belongs to the Special Issue Reviews on Reproductive Biology and Medicine)
►▼
Show Figures
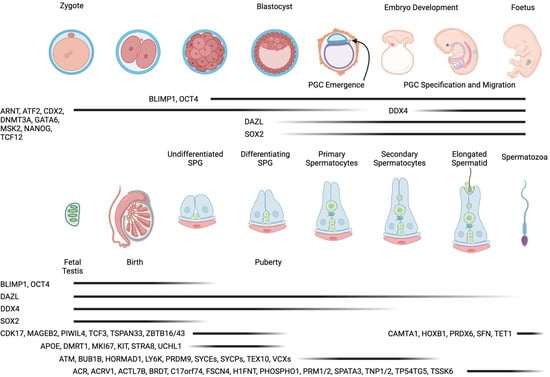
Figure 1
Open AccessEditorial
Special Issue Featuring Papers for Celebrating the Third Year since the Founding of Reproductive Medicine
by
Stefano Palomba
Reprod. Med. 2023, 4(3), 210-214; https://doi.org/10.3390/reprodmed4030019 - 6 Sep 2023
Abstract
It is a great pleasure to introduce this Special Issue celebrating the third year since the founding of Reproductive Medicine [...]
Full article
Open AccessArticle
Relationship between Ovarian Reserve Markers and Body Mass Index in Infertile Women with and without Polycystic Ovary Syndrome: A Retrospective Case–Control Study
by
Luisa Casadei, Ilaria Nacci, Veronica Vicomandi, Roberto Pietro Sorge and Carlo Ticconi
Reprod. Med. 2023, 4(3), 198-209; https://doi.org/10.3390/reprodmed4030018 - 17 Aug 2023
Abstract
This study, carried out on 94 women with polycystic ovary syndrome (PCOS) and 176 controls without it, investigated the influence of body mass index (BMI) on serum levels of antimüllerian hormone (AMH), follicle stimulating hormone (FSH), luteinizing hormone (LH), and 17ß-estradiol (E2) in
[...] Read more.
This study, carried out on 94 women with polycystic ovary syndrome (PCOS) and 176 controls without it, investigated the influence of body mass index (BMI) on serum levels of antimüllerian hormone (AMH), follicle stimulating hormone (FSH), luteinizing hormone (LH), and 17ß-estradiol (E2) in infertile patients. Patients were assigned to four subgroups according to age (<35 or ≥35 years) and BMI (<25 kg/m2 or ≥25 kg/m2). Significant differences between PCOS-affected and control women were observed with respect to most of the parameters of interest. In both PCOS-affected and control women, age was inversely correlated with AMH. In the control patients, age was directly correlated with FSH and LH. In women affected by PCOS, no correlation was found between BMI and serum levels of AMH, E2, and LH, except FSH. No correlation was found between BMI and markers of ovarian reserve in control women. BMI was not correlated with AMH in any of the four subgroups considered regardless of the presence of PCOS. An inverse correlation was found only in PCOS-affected women aged ≥35 years between a BMI < 25/FSH and a BMI ≥ 25/LH. The possible association between BMI and ovulation disorder (OD) was investigated in 96 control women aged ≤37 years. In women with OD, the BMI values were significantly higher and FSH and E2 levels were lower than those of patients without OD. Taken together, our data suggest that BMI is not related to hormonal parameters of ovarian reserve, irrespective of the presence of PCOS, and could influence ovulation disorder rather than cause a decrease in ovarian reserve.
Full article
(This article belongs to the Special Issue Feature Papers in Celebration of the Fourth Anniversary of the Founding of Reproductive Medicine)
Open AccessReview
The Management of Inflammatory Bowel Disease during Reproductive Years: An Updated Narrative Review
by
Nariman Hossein-Javaheri, Michael Youssef, Yaanu Jeyakumar, Vivian Huang and Parul Tandon
Reprod. Med. 2023, 4(3), 180-197; https://doi.org/10.3390/reprodmed4030017 - 3 Aug 2023
Cited by 1
Abstract
Inflammatory bowel disease (IBD) frequently affects women of childbearing age and often coincides with pregnancy. With an increased incidence of IBD, gastroenterologists and obstetricians are more frequently involved in caring for women of reproductive age. While the development of novel therapies has allowed
[...] Read more.
Inflammatory bowel disease (IBD) frequently affects women of childbearing age and often coincides with pregnancy. With an increased incidence of IBD, gastroenterologists and obstetricians are more frequently involved in caring for women of reproductive age. While the development of novel therapies has allowed for successful conception and pregnancy outcomes, many patients may hesitate to conceive due to concerns for presumed adverse IBD effects on maternal and fetal health. As such, a noticeable percentage of patients may choose voluntary childlessness. Indeed, active IBD carries a greater risk of adverse pregnancy outcomes, including a loss of pregnancy, preterm delivery, and emergent C-sections. However, those with a quiescent disease tend to have fewer pregnancy complications. Therefore, it is essential to achieve remission prior to conception to optimize pregnancy outcomes. Dedicated IBD and pregnancy clinics can greatly assist in improving patient knowledge and attitudes towards pregnancy; through individualized pre-conception counseling, education, and medication adherence, the risks of poor pregnancy outcomes can be minimized. Furthermore, it is important for healthcare providers to have a sufficient understanding of the medication safety and tools to measure the disease activity, while counseling patients during gestation and breastfeeding periods. This review article aims to provide the most recent evidence-based management methods for IBD during pregnancy.
Full article
(This article belongs to the Special Issue Reviews on Reproductive Biology and Medicine)
Open AccessArticle
Travel during Pregnancy: A Web-Based Survey of People Who Have Been Pregnant within the Past 10 Years
by
Lada H. Nechval and Kathleen M. Antony
Reprod. Med. 2023, 4(3), 166-179; https://doi.org/10.3390/reprodmed4030016 - 28 Jul 2023
Abstract
►▼
Show Figures
Travel is frequent among many populations, including pregnant people. The focus of this online survey was to better understand the travel practices of people who have been pregnant within the last ten years. An online survey was conducted for three months through social
[...] Read more.
Travel is frequent among many populations, including pregnant people. The focus of this online survey was to better understand the travel practices of people who have been pregnant within the last ten years. An online survey was conducted for three months through social media posts on Facebook and Twitter. Previously pregnant people were asked questions about where they traveled, if they cancelled any travel plans, and travel-related discussions with their obstetric provider. During the three months the survey was open, 469 participants completed the survey. A total of 390 (83.2%) participants traveled domestically, while 114 (24.3%) traveled internationally or between non-contiguous states within the United States of America (USA). Of these respondents, 170 (44.2%) of the domestic travelers and 69 (61.1%) of the international travelers reported discussing travel plans with their OB provider. Additionally, 49 (10.5%) participants cancelled at least one domestic trip and 30 (6.41%) cancelled at least one international trip. Regarding travel discussions, 6 (3.6%) participants who traveled domestically and 2 (2.9%) who traveled internationally reported that their OB provider initiated the conversation. Many pregnant people choose to travel domestically and internationally. However, it is also clear that not all travelers discuss plans with their OB provider, and in few cases does the provider initiate the conversation. Given the frequency with which people travel, pregnant people and their OB providers should have conversations regarding travel to minimize potential risks.
Full article

Figure 1
Open AccessReview
The Duration of Menstrual Blood Loss: Historical to Current Understanding
by
Marwan Habiba and Giuseppe Benagiano
Reprod. Med. 2023, 4(3), 145-165; https://doi.org/10.3390/reprodmed4030015 - 26 Jul 2023
Cited by 2
Abstract
Most published research focuses on the amount of menstrual blood loss and, to a lesser extent, on cyclicity. Little attention has been paid to the duration of bleeding, the factors that enable its cessation within a ‘normal’ timeframe, or to patterns that entail
[...] Read more.
Most published research focuses on the amount of menstrual blood loss and, to a lesser extent, on cyclicity. Little attention has been paid to the duration of bleeding, the factors that enable its cessation within a ‘normal’ timeframe, or to patterns that entail interruption and resumption of blood loss. The definition of what constitutes normal remains arbitrary and there is no therapy specifically designed to shorten the duration of bleeding. Here, we critically review the literature that addresses the duration of bleeding and the factors that trigger endometrial breakdown and repair. Available reports used population averages which mask inter- and intra-individual variations. The duration of bleeding is not necessarily linked to the amount of loss but may be influenced by age, ethnicity, habitus, region and altitude of residence, dieting and stress. The onset of bleeding has been linked to declining steroid production by the corpus luteum. There remains considerable controversy around the extent of endometrial shedding at menstruation. This is likely to vary within and between women. The significance of a change from previous patterns, very short or prolonged bleeding, days of light loss or spotting before or after days of bleeding, or of bleed-free days that punctuate flow, remain poorly understood.
Full article
Highly Accessed Articles
Latest Books
E-Mail Alert
News
Topics
Topic in
Biomedicines, CIMB, Endocrines, IJMS, JMP, Life, Reprod. Med.
Pathogenesis of Pregnancy-Related Complications 2.0
Topic Editors: Ilona Hromadnikova, Katerina KotlabovaDeadline: 31 August 2024

Conferences
Special Issues
Special Issue in
Reprod. Med.
Feature Papers in Reproductive Medicine 2024
Guest Editor: Berthold HuppertzDeadline: 31 December 2024
Special Issue in
Reprod. Med.
Advances in Reproductive Toxicology—2nd Edition
Guest Editor: Giulia GuerrieroDeadline: 31 January 2025
Topical Collections
Topical Collection in
Reprod. Med.
Recent Advances in Preeclampsia
Collection Editor: Berthold Huppertz
Topical Collection in
Reprod. Med.
Reproductive Medicine in Europe
Collection Editor: Simone Ferrero






